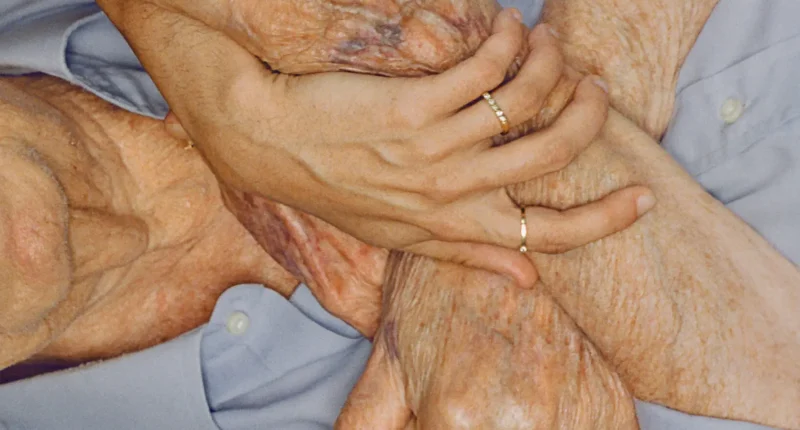
My 7-year-old son, Carl, realized that it was Tuesday and asked why Robert was not coming to our house that day. Robert had been a caregiver for my husband, Ady Barkan, for more than five years, helping with Ady’s day-to-day activities as he became progressively paralyzed because of the neurodegenerative disease amyotrophic lateral sclerosis, or A.L.S.
Tuesdays were Robert’s days, when he would help Ady work during the day and pick up Carl and his sister, Willow, in the afternoon, often going out for an activity in our red wheelchair-accessible van. Robert also helped Ady get into bed four nights a week, arriving around the kids’ bedtime and staying until 10 p.m.
Ady died from complications of A.L.S. in early November. Since then, the bustle of caregivers around our house has been strangely suspended for the first time in years.
The kids didn’t understand why Robert couldn’t come anyway, so I texted to invite him for dinner. We had our usual Tuesday meal of tacos, which Ady had branded “Taco Martes”; while I cooked, Carl, Willow and Robert played Uno in the living room.
Ady and I had close relationships with his caregivers, many of whom worked with us for years. They allowed Ady to continue to live in our home, surrounded by his family, even after his paralysis had progressed to the point where I could not care for him on my own.
It’s likely that most A.L.S. patients do not have access to this kind of support — or to adequate caregiving in general. Health insurance plans cover little, if any, in-home caregiving to assist with the tasks of daily life (as opposed to skilled nursing services, which administer medicines and change bandages, for example). Medicare also does not cover assistance with activities like bathing and dressing. To qualify for Medicaid — which varies state by state and has lengthy wait lists for home care — patients and their families usually must exhaust almost all of their assets first, which would have left me, as a now 39-year-old widow, with almost no savings. We were fortunate to arrive at an ad hoc arrangement with our health insurance company that reimbursed most of Ady’s caregiving costs, which totaled about $40,000 a month for round-the-clock care.
You read that right — by the end of his life, we paid nearly half a million dollars a year for Ady’s care. Living with A.L.S. offers an extreme example of the care crisis that the United States is facing right now. Private caregiving is exorbitantly expensive, even as more Americans will need paid care in the coming years. The pandemic revealed how much our society relies on caregivers, but we have failed to make changes to our insufficient caregiving system. Political action to make home care more affordable and available seems to have stalled in our divided Congress.
We cannot accept this status quo. In this election year, candidates will present their platforms to voters. We have the opportunity to push those seeking office to prioritize a care agenda that would recognize the importance of caregiving to millions of people’s lives. We can ask how they will support patients and caregivers so that more people can enjoy the quality of life that Ady’s caregivers made possible.
Ady was diagnosed with A.L.S. in 2016, when Carl was 4 months old. In 2019, he underwent a tracheotomy, which inserted a tube into his windpipe so that a ventilator could breathe for him. A tracheotomy turns A.L.S. from a terminal illness into a long-term condition, but it also requires constant maintenance: suctioning secretions, changing the tubing and responding to any alarms on the ventilator. Because Ady was paralyzed and could not perform these actions himself, he needed 24/7 caregiving support provided by a team of nine caregivers, including Robert.
Early in Ady’s illness, he and I had resisted hiring caregivers, wanting to hold on to our normal life and fearing that having strangers in our home would be too intrusive. But once we reached the stage when we needed additional help, it turned out that having it allowed a little normalcy back into our lives. He and I could be partners again, rather than patient and caregiver. We could relax, chat and watch TV in the evenings, instead of my going through an hourslong routine — after putting our children to sleep first — to get him ready for bed. To be candid, hiring caregivers saved our marriage.
But because of the high cost of private caregiving, most people with A.L.S. face a choice: They can live in a nursing home, funded by Medicare, Medicaid or private insurance; they can rely on family caregivers, who must then often leave their jobs to provide full-time care; or they can elect to die by physician-assisted suicide. Most simply cannot access or afford the round-the-clock caregiving that is necessary for someone with the disease and others like it.
The need for long-term caregiving is not unique to those with A.L.S. The U.S. Department of Health and Human Services has found that 70 percent of people over 65 need long-term services and support, and that those needs are concentrated in poorer households. Yet only about 3 to 4 percent of Americans over age 50 have long-term care insurance. A 2019 report published by the Department of Health and Human Services found that 48 percent of people over 65 received some paid care, but many relied on family and other unpaid caregivers. Medicare generally does not cover long-term care, and more than 650,000 people are on Medicaid waiting lists or interest lists for home and community-based services. As the current population continues to age, more people will need long-term care than ever before.
The care crisis also directly affects caregivers, who are overworked, underpaid and underappreciated. The median wage for a direct care worker was $15.43 an hour in 2022, meaning that many caregivers live in poverty and rely on public assistance. The work can be exhausting and difficult, with many caregivers working multiple part-time jobs. However, we often devalue this work by thinking of in-home caregivers as “help” rather than as medical professionals.
Because we hired private caregivers, Ady and I were able to offer them benefits such as paid sick days and a severance package when he died. His caregivers earned a living wage based on the specialized skills required for different aspects of the job. Early in his career, Ady helped write the legislation guaranteeing workers in New York City paid sick leave, and he was determined to make caregiving a stable, sustainable career. Because training new caregivers could take weeks or months, it was crucial for him to have a reliable crew.
On Sept. 8, 2021, Ady wrote in these pages about the benefits that his caregivers brought to his life and called on the president and Congress to fund home care. Despite branding caregivers as “essential workers” during the pandemic, we have failed to make any changes to our insufficient caregiving system.
In 2022, a proposed $150 billion in funding for Medicaid home and community-based services, or H.C.B.S., was stripped from President Biden’s Build Back Better legislation. When the reformulated Inflation Reduction Act finally passed, it did not include funding for H.C.B.S. But the urgency of the problems has not diminished and we must continue to call on elected officials to act.
Officials have proposed legislative solutions to some shortcomings of our current system. The Better Care Better Jobs Act bill, introduced into Congress last January, would expand eligibility for home and community-based services, such as in-home caregiving, for millions of people. It would also increase wages and benefits and help caregivers organize, making these jobs more appealing and secure.
Another bill, the H.C.B.S. Access Act, introduced last spring, would make H.C.B.S. coverage mandatory under Medicaid for all eligible people, helping them move off waiting lists, as well as strengthen wages and support for caregivers.
Neither proposal advanced out of committee, even though Americans are largely in favor of policies that support paid and unpaid caregiving. Support for caregiving is bipartisan, but funding it has unfortunately become a partisan football, tossed back and forth in our increasingly dysfunctional Congress. But caregiving is a way of life — a necessity imposed upon many people who cannot afford paid caregivers, but also a beautiful expression of love and community. Just as having caregivers in our home allowed us to feel more like a family, so too can caregiving be both a burden and a blessing. It was one of the most profound experiences of my life to care for Ady as he became progressively disabled, but I could not have done it without the caregivers, teachers, babysitters, friends and family who have cared for Ady, our children and me over the years.
Now that Ady is gone, I know that one of the most beautiful aspects of his awful disease was this community of care that we created around him. Far from disrupting our privacy, the caregivers and other friends and family who supported us through Ady’s illness allowed us to live in a more communal way — one that Americans often idealize while finding it difficult to achieve. Rather than living in a traditional nuclear family, my children live surrounded by many loving adults who contribute to their care.
Ady believed in a world where sick and disabled people were not isolated in their homes or segregated in skilled nursing facilities, and where caregiving was a career that offered dignity and financial stability. As he frequently noted, it is unconscionable that the richest nation in the world refuses to provide this basic social safety net for its citizens — to fulfill the moral obligation of allowing people to maintain a sustainable quality of life that recognizes their full humanity. After Ady’s death, leaders from across the government and public policy commemorated his activism. One way to honor his legacy is to make sure that everyone has access to the high quality care that brought joy and contentment to the last few years of his life.